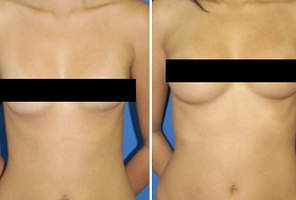
Gynecomastia is a medical term that refers to excess amounts of fat or breast tissue in the chest or breast region in men. This condition is fairly common as it affects an estimated 40 to 60 percent of men. The condition is relatively common in adolescent boys, and in most cases in this age group, symptoms disappear in a matter of months. It may affect only one breast or both.
Potential Causes:
- Puberty
- Steroid abuse
- Obesity
- Tumors
- Genetic disorders
- Chronic liver disease
- Side effects of many medications
- Castration
- Klinefelter Syndrome
- Gilbert's Syndrome
- Aging
Various drugs may contribute to gynecomastia, such as:
- Estrogens or drugs with estrogen-like activity such as diethylstilbestrol, digoxin, phytoestrogens, estrogen-contaminated food and estrogen-containing cosmetics.
- Drugs that enhance estrogen production such as gonadotropins, clomiphene, phenytoin, and testosterone.
- Drugs that inhibit testosterone synthesis or action such as ketoconazole, flagyl, cisplatin, spironolactone, zantac, flutamide, finasteride, and etomidate.
- Drugs that act by unknown mechanisms such as isonicotinic acid hydrazide, methyldopa, busulfan, tricyclic antidepressants, valium, penicillamine, omeprazole, phenothiazines, calcium channel blockers, ACE inhibitors, alcohol, marijuana, and heroin.
In cases of obesity, weight loss can alter the condition and minimize overall body fat levels which can minimize excess fat in the chest. Cessation of medication that may be linked to excess fat and tissue in the chest may or may not cause reversal of gynecomastia. For all other causes, surgery is the only known physical remedy. Male breast reduction removes fat and or glandular tissue from the breasts and in extreme cases removes excess skin, resulting in a chest that is flatter, firmer, and contoured to patient satisfaction.
Who is a candidate for Male Breast Reduction?
Surgery to correct gynecomastia can be performed on healthy, emotionally stable men of any age. The best candidates for surgery have firm, elastic skin that will reshape to the body's new contours.
Prior to surgery, weight loss, diet and lifestyle changes, and other alterations are encouraged to ensure that all possible solutions have been considered. Individuals who drink alcoholic beverages in excess, smoke marijuana, or consume anabolic steroids are usually not considered good candidates for surgery since lifestyle alterations could readily alter excess fat and tissues in the chest area. Therefore, patients are first directed to stop the use of these drugs to see if breast fullness will diminish before surgery is considered an option.
What are the risks and complications of the procedure?
Risks include infection, skin injury, excessive bleeding, adverse reaction to anesthesia, and excessive fluid loss or accumulation. The procedure may also result in noticeable scars, permanent pigment changes of the surgery area, or slightly mismatched breasts or nipples.
Asymetry may also be a concern, and if asymmetry is significant, a second procedure may be performed to remove additional tissue.
Breast reduction can cause loss of breast sensation or numbness, which may last up to a year or more.
This is not an exhaustive list of possible risks and an in-depth discussion with a professional and experienced cosmetic surgeon, as well as personal research, is important to fully understand the procedure.
What is needed to prepare for Male Breast Reduction and how is the procedure performed?
Prior to diagnosis and treatment, the treating cosmetic surgeon will need complete medical history records. First, the surgeon will examine the chest area and check for causes of gynecomastia, such as impaired liver function, use of estrogen-containing medications, or anabolic steroids. If a medical problem is suspected, you'll be referred to an appropriate specialist.
A mammogram, or breast x-ray, may also be recommended if anything suspect is found within the tissue to help diagnose the cause. This will not only rule out the very small possibility of breast cancer, but will reveal the composition of the tissue in the area. Once the surgeon knows how much fat and glandular tissue is contained within the unwanted tissue, the necessary surgical approach can be recommend.
Smokers should plan to stop smoking for a minimum of one or two weeks before surgery (longer ideally) and during recovery. Smoking decreases circulation and interferes with proper healing. Directly following post-operative care requirements is important for a healthy and satisfactory recovery.
If excess glandular tissue is the primary cause of breast enlargement, it will be removed. The excision may be performed alone or in conjunction with liposuction to help remove excess fat. In a typical procedure, an incision is made in a barely visible location, such as the edge of the areola, or in the under arm area. Working through the incision, the surgeon removes excess glandular tissue, fat and skin from around the areola and from the sides and bottom of the breast. Major reductions that involve the removal of a significant amount of tissue and skin may require larger incisions that result in more obvious scars. If liposuction is used to remove excess fat, the cannula is usually inserted through the existing incisions. Each patient has unique needs and every procedure is different and tailored to the patient.
If the cause of gynecomastia consists primarily of excessive fatty tissue rather than glandular tissue, liposuction may be all that's needed to remove the fat. A small incision, less than a half-inch in length, is made around the edge of the nipple or in the underarm area to insert a cannula which assists with the breakdown and removal of body fat.
A small drain may be inserted through a separate incision to help with the removal of excess fluids which accumulate during surgery. Once closed, the incisions are usually covered with a dressing. The chest may be wrapped to keep the skin firmly in place and post-operative care begins.
What is recovery like?
Whether excision only, liposuction, or a combination of both have been used, patients will experience bruising, swelling, and discomfort for a few days after surgery. Discomfort can be controlled with prescribed medications.
To help reduce swelling, an elastic pressure garment worn continuously for a week or two, and for a few weeks longer at night, will be recommended. Although swelling gradually dissipates in the first few weeks, it may be three months or more before the final results of the surgery are apparent.
Patients are often encouraged to begin walking around on the day of surgery, and can return to work when well enough--which could be as early as a day or two after surgery. Any stitches will generally be removed about 1 to 2 weeks following the procedure. Each patient's recovery time is unique and this should be considered as the body adjusts and heals.
Avoiding heavy exercise for about three weeks is important for recovery. Any physical activity that puts the surgery site at risk in anyway should be avoided for at least a month. A month generally must pass before normal activities can safely resume.
To promote ideal healing, avoiding sun exposure where scars appear for at least six months is important. Sunlight can permanently affect the skin's pigmentation, causing the scar to turn dark. If sun exposure is unavoidable, use a strong sunblock.
The results of the procedure are significant and permanent, yet each patient is unique and results will vary. Realistic expectations increase satisfaction, as well as proper knowledge of the procedure, thoroughly discussing options and risks with a cosmetic surgeon, and following guidelines to support a safe and quick recovery time.
Disclaimer: This information is intended only as an introduction to this procedure. This information should not be used to determine whether you will have the procedure performed nor does it guarantee results of your elective surgery. Further details regarding surgical standards and procedures should be discussed with your physician.
By OnlineSurgery Staff & Dunya Atisha, M.D.
Updated: November 13, 2008